TL;DR:
- Personalized health strategies tailor interventions using individual genetic, behavioral, and environmental data.
- Advanced diagnostics and AI analysis improve outcomes like weight management, energy, and sleep quality.
- Ongoing monitoring and adaptation are essential due to biological variability and life stage changes.
Generic health advice is everywhere, yet most people following it still struggle with low energy, poor sleep, and metabolic drift. The reason is not a lack of effort. It is that general recommendations are built for populations, not for you. Personalised nutrition significantly outperforms one-size-fits-all interventions across key health outcomes, including weight, mood, and metabolic markers. Targeted health strategies use your unique biology as the starting point, not an afterthought. This article explains what those strategies involve, which technologies power them, what results you can realistically expect, and where the genuine limitations lie.
Table of Contents
- What are targeted health strategies?
- The science and technology behind personalisation
- How personalised strategies improve energy, resilience, and wellness
- Caveats and challenges with targeted health strategies
- A fresh perspective: what most people get wrong about targeted health
- Take the next step towards personalised wellness
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Personalisation works | Tailored strategies reliably outperform ‘one-size-fits-all’ health advice in improving key outcomes. |
| Diagnostics empower you | Tools like CGM and biomarkers enable truly bespoke recommendations for nutrition and wellness. |
| Benefits extend beyond weight | Energy, mood, sleep, and resilience all improve measurably with personalisation. |
| Science still evolves | Expert guidance and continual review are essential as methods and technologies rapidly advance. |
What are targeted health strategies?
Targeted health strategies are not simply a more detailed version of standard wellness advice. They represent a fundamentally different model. Rather than applying population-level guidelines to an individual, they use your specific genetic profile, behavioural patterns, and environmental context to shape every recommendation. Targeted health strategies tailor interventions using an individual’s genetic, behavioural, and environmental information to improve efficacy in ways that generic protocols cannot match.
The contrast with conventional advice is stark. Standard guidance tells you to eat more vegetables, sleep seven to nine hours, and exercise regularly. These are not wrong, but they are incomplete. Two people following identical advice can produce entirely different physiological responses because of differences in gut microbiome composition, hormonal rhythms, insulin sensitivity, and stress reactivity. Personalised strategies account for this variation from the outset.
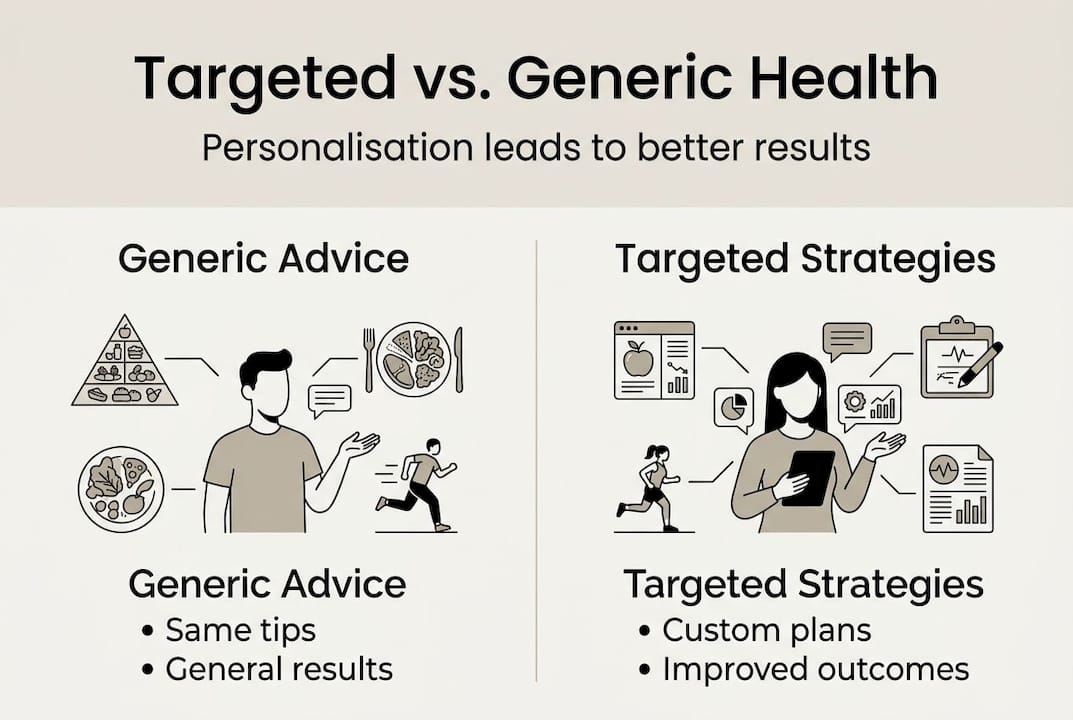
You can explore the broader framework behind this approach in our precision health overview, which sets out how individual biological data translates into actionable protocols.
Here is what distinguishes targeted strategies from conventional wellness advice:
- They use measurable biological data rather than population averages
- They adapt over time as your physiology and circumstances change
- They identify root causes rather than managing surface-level symptoms
- They prioritise interventions with the highest predicted impact for your specific profile
- They quantify outcomes so progress is trackable, not assumed
“The most powerful health intervention is not the most popular one. It is the one calibrated precisely to the individual receiving it.”
This shift from generic to targeted is not a luxury reserved for elite athletes or research participants. It is increasingly accessible, and the evidence base supporting it is growing rapidly. The question is no longer whether personalisation works. It is how to apply it effectively to your own biology.
The science and technology behind personalisation
Personalised health strategies are only as good as the data underpinning them. Fortunately, the tools available in 2026 are considerably more powerful than they were even five years ago. Modern personalisation relies on genomic sequencing, biomarker identification, pharmacogenomics, artificial intelligence, and multi-omics integration to refine individual risk and treatment pathways.
Genomic sequencing reveals inherited predispositions, including how efficiently you metabolise certain nutrients, your risk profile for inflammatory conditions, and how your body responds to specific exercise stimuli. Biomarker analysis goes further by capturing what is actually happening in your body right now, not just what your genes suggest might happen. Understanding how to interpret this data is covered in depth in our guide to analysing biomarkers.
Artificial intelligence ties these data streams together. Machine learning models can identify patterns across thousands of variables simultaneously, surfacing correlations that no clinician could spot manually. The role of data-driven diagnostics in translating raw numbers into prioritised recommendations is central to this process.
| Technology | What it measures | Clinical value |
|---|---|---|
| Genomic sequencing | Inherited risk, nutrient metabolism | Long-term disease prevention |
| Continuous glucose monitor | Real-time glucose response | Metabolic optimisation |
| Multi-omics panels | Proteome, metabolome, microbiome | Systemic health mapping |
| PhenFlex challenge | Phenotypic flexibility under stress | Recovery and resilience capacity |
| AI integration | Cross-variable pattern recognition | Personalised protocol refinement |
Pro Tip: A single biomarker result tells you very little in isolation. The value comes from tracking trends across multiple markers over time and correlating them with lifestyle inputs. That is where the real signal emerges.
The role of AI in personalisation is not to replace clinical judgement but to augment it, processing data at a scale and speed that makes truly individualised protocols feasible for anyone, not just research cohorts.
How personalised strategies improve energy, resilience, and wellness
The technologies described above are not academic exercises. They produce measurable, real-world changes in how you feel and function. Continuous glucose monitoring, health space modelling, and PhenFlex testing precisely measure phenotypic flexibility, giving clinicians a detailed picture of how well your body adapts to metabolic stress and where its limits lie.

Phenotypic flexibility is the body’s capacity to mount and recover from physiological challenges. It is a strong predictor of long-term resilience and disease resistance. When you measure it directly, you can design interventions that specifically expand that capacity rather than guessing at what might help.
The outcomes data is compelling. Personalised nutrition produced greater weight loss, lower triglycerides, improved mood, better sleep, and higher energy levels compared to standard dietary guidelines in the ZOE trial. These are not marginal gains. They represent meaningful improvements in daily quality of life.
Practical benefits reported by individuals following targeted protocols include:
- Sustained energy across the day without reliance on stimulants
- Faster recovery from physical and cognitive exertion
- Improved sleep architecture, particularly deep sleep duration
- Reduced inflammatory markers within eight to twelve weeks
- Greater metabolic flexibility, meaning the ability to efficiently use both glucose and fat as fuel
You can see how health monitoring tools like continuous glucose monitors fit into a broader wellness protocol, and how a personalised nutrition guide translates these findings into daily food decisions. For a deeper look at the metabolic dimension, our data-driven metabolic health resource sets out the key markers worth tracking.
| Outcome | Standard advice | Personalised strategy |
|---|---|---|
| Weight management | Modest, inconsistent | Greater and sustained |
| Energy levels | Variable | Consistently improved |
| Sleep quality | Minimal change | Measurable improvement |
| Triglycerides | Slight reduction | Significantly lower |
| Mood stability | Unreliable | Notably better |
Caveats and challenges with targeted health strategies
Targeted health strategies are not infallible, and treating them as such is a mistake. Patient-specific interventions sometimes produce variable effects and require flexible, evidence-based review rather than fixed protocols applied indefinitely. Biology changes. Life circumstances shift. What works at thirty-five may need recalibrating at forty-five.
Here are the key limitations every health-conscious individual should factor in:
- Individual variation is real. Even with comprehensive data, some people respond unexpectedly to interventions. Ongoing monitoring is essential, not optional.
- Timing and life stage matter. Hormonal shifts, ageing, pregnancy, and periods of high stress all alter how your body responds to the same inputs. Protocols must adapt accordingly.
- Access is not equal. Advanced diagnostics carry a cost, and not everyone can access them. This creates a health equity gap that the field has not yet resolved.
- Data without interpretation is noise. More testing does not automatically mean better outcomes. The value lies in expert synthesis of what the data means for your specific situation.
- Validation is ongoing. Many multi-omics applications are still being refined. Responsible use means staying within evidence-supported boundaries and avoiding premature conclusions.
Pro Tip: Treat your personalised health protocol as a living document, not a fixed prescription. Schedule a formal review every three to six months and adjust based on new data, not just how you feel.
“Precision health is not about perfection. It is about progressively reducing uncertainty through better data and smarter interpretation.”
The ethical dimension matters too. As AI and multi-omics scale, questions around data privacy, algorithmic bias, and equitable access become increasingly urgent. Responsible personalisation means engaging with these questions, not ignoring them. Our resource on transforming precision health addresses how data-driven approaches can be applied responsibly and sustainably.
A fresh perspective: what most people get wrong about targeted health
The most common misconception we encounter is that more data automatically equals better health outcomes. It does not. Data is only useful when it is interpreted within the right context, acted upon consistently, and reviewed as circumstances evolve. Collecting extensive test results and then applying them rigidly is not personalisation. It is just expensive guesswork.
The second misconception is that targeted health is a one-time intervention. Run the tests, get the protocol, follow it forever. In reality, the most valuable gains come from iterative refinement. Your biology is not static, and your strategy should not be either.
What genuinely moves the needle is the combination of high-quality diagnostics, expert synthesis, and adaptive application over time. The AI health trends shaping precision medicine in 2026 point clearly in this direction: integration, not accumulation, is the key. More tests without better interpretation will not close the gap between where you are and where you want to be. Fewer, better-chosen interventions reviewed regularly will.
Take the next step towards personalised wellness
If the evidence in this article has shifted how you think about your health, the logical next step is to act on it with data rather than guesswork.
At AI Healthician, we offer a range of advanced diagnostics designed to give you the biological clarity that generic advice never can. Whether you want to start with DNA health testing to understand your genetic predispositions, assess your metabolic capacity with an active metabolic test, or establish your baseline with a resting metabolic analysis, each test feeds into a personalised protocol built around your actual physiology. This is where the shift from knowing to doing begins.
Frequently asked questions
How are targeted health strategies different from general wellness advice?
Targeted health strategies use your unique genetics, behaviours, and advanced diagnostics to deliver tailored recommendations, unlike generic advice which applies the same tips to everyone. Personalised medicine tailors interventions to the individual, improving efficacy in ways population-level guidance cannot.
What types of technologies are used for personalising health?
Technologies include genomic sequencing, AI-driven data analysis, continuous glucose monitors, and biomarker testing to uncover tailored interventions. Genomic and AI tools are now central to building precise, individual health protocols.
Are personalised health strategies suitable for everyone?
Most individuals benefit from some degree of personalisation, but effectiveness varies by age, life stage, and individual differences. Dynamic adaptation is essential because timing and patient-specific factors significantly influence results.
What results can I expect from following a targeted health plan?
Empirical studies show better weight, mood, sleep, and metabolic outcomes compared to standard plans when using personalised strategies. Personalised nutrition led to superior health outcomes versus general dietary guidelines in controlled trials.
What are the main limitations of targeted health strategies?
Challenges include complex validation requirements, possible equity gaps, and the need for continuous data review as science evolves. Empirical validation remains essential, and access gaps mean not everyone benefits equally from current precision health tools.



 matt@aihealthician.co.uk
matt@aihealthician.co.uk








